
Bringing home a baby who has spent time in the Neonatal Intensive Care Unit (NICU) either as a result of premature birth or a low birth weight feels amazing as your dream of finally being together and starting your lives as a family come true. However, leaving the “safety and security” of being in the NICU and coming home without all the monitors and machines can be a huge adjustment. Especially as parent’s are often left with little advice from the medical staff regarding precautions around safe sleep practices for these little babies.
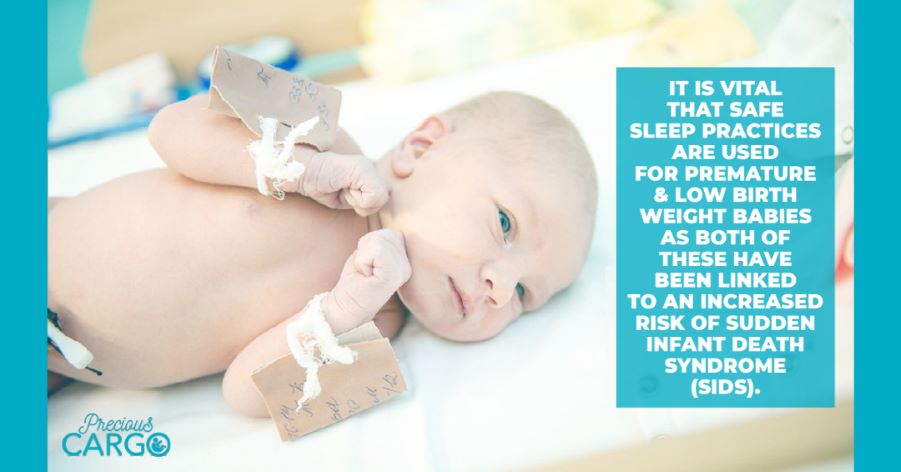
It is vital that safe sleep practices are used for premature and low birth weight babies as both of these have been linked to an increased risk of Sudden Infant Death Syndrome (SIDS). To reduce this possibility, you should place your baby on a firm and flat mattress on their back for every sleep. It is also recommended that you share the same room as your baby for at least the first 6 months.
It may feel as though your baby has been in the NICU for a lifetime and yet simultaneously you feel like you are completely unprepared to bring them home. The best way to alleviate these concerns is to provide yourself with accurate information.
What is considered a premature baby?
A baby who is born before 37 weeks of gestation is considered premature. The range of prematurity extends from late preterm babies where a baby is born between 34 and 36 weeks all the way to extremely preterm babies where a baby is born before 28 weeks. While health concerns are perhaps not as critical in late preterm babies when compared to very preterm babies, late preterm babies still have a higher risk of health problems than a baby born at full term. They are also more likely to be of low birth weight.
Interestingly, the most recent statistics released in South-Africa show that the number of premature births have increased over the years with 1 in 7 babies now born before 37 weeks. While the chances of having a premature baby may seem high, they are greatly reduced when you receive the recommended medical care. Contributing factors to preterm labour such as high blood pressure, diabetes, infection and a weak cervix are more likely to be picked up early enough to treat should you receive prenatal care.
What defines a baby as low birth weight?
An average healthy weight for a new-born baby is approximately 3.5kg. As with prematurity, there is a range of low birth weights extending from a general low birth weight of less than 2.5kg to an extremely low birth weight of 1kg.
Unfortunately, due to various factors a baby may not grow as expected and be smaller at birth. There are generally two main causes as to why a baby would be born with a low birthweight:
-
Premature birth
A baby who is born too early has less time to fill out and gain weight. The earlier a baby is born, the lower their birth weight would be. -
Fetal growth restriction
This is when a baby does not gain the expected amount of weight each week. The cause of it varies as well as ways to handle it. It is detected by your doctor and often results in more frequent ultrasounds and closer monitoring.

Is there an increased risk of SIDS for premature or low birth weight babies?
The risk of SIDS for a baby who was born prematurely or who was born with a low birth weight is up to four times higher when compared to those who were born at full term. This risk is higher the earlier the baby is born or the lower their birth weight is.
One of the proposed suggestions as to why there is an increased chance of SIDS in premature and low birth weight babies is that a baby who is born prematurely has not had as much time for their brain to mature. This means that they may have less control over unconscious processes such as breathing and maintaining their heart rate.
What safe sleep principals should I follow when my baby comes home?
As a parent sitting in the NICU you begin to find comfort in the constant beeping of a heart rate monitor and going home without that continuous reassurance can be daunting. Knowing that you are making use of safe sleep practices is one step closer to reducing the chance of SIDS.

- Placing your baby on their back
- This is also true for babies who still receive oxygen when they come home
- On a firm and flat mattress with a waterproof covering
- Alone in their cot with no loose items around them
- Sharing a room with your baby for at least the first 6 months
- It is important that this not be confused with sharing a bed with them. (Read our co-sleeping blog here)
- Often a Moses basket or bassinet is the easiest way to achieve this
What other safe sleep precautions should I have in place when my baby comes home?
Along with the importance of your baby sleeping alone and flat on their back, other factors which can assist in reducing the risk of SIDS have been identified. These include:
Room temperature:
One of the contributing factors which can increase the risk of SIDS is overheating. While in the NICU, your baby’s body temperature would have been continuously monitored by one of the cables attached to them ensuring that they did not overheat. This is not possible to do once you are home.

Therefore the easiest way to prevent overheating is by maintaining your baby's room at an ideal temperature of 20℃- 22℃. Read our article on Safe Sleeping Temperatures for babies for more information about safe sleeping temperatures.
Clothing:
Hand in hand with making sure that your baby does not overheat is the amount of clothing they have on. The easiest way to ensure that they do not get too hot or cold is to dress them in layers as this makes it easier for you to add or remove items depending on the temperature of the room. While your baby likely wore a hat in the NICU, it is recommended that you not do this when they are home and inside. Babies release heat from their heads and if they are wearing a hat they are unable to do that. To find out more about clothing recommendations and preventing overheating, read our article on Safe Sleeping Temperatures for babies.


Monitoring devices:
Although monitoring devices such as audio, visual and movement monitors are not recommended by the American Academy of Paediatrics’, they may help ease fears of knowing if your baby has stopped breathing.
The main reason for the hesitation of using these monitors is that a parent may rely solely on them as a way to monitor their baby and not check on their baby as often. However, if these monitors are used along with the safe sleep practices of your baby sleeping alone on their back on a firm and flat mattress in an empty cot in the same room as you then they may add additional value. Movement monitors such as the Suza which attaches to your baby’s nappy are designed specifically to alert you should it not register movement after a certain amount of time. This can add an extra layer of reassurance for you. Read our blogs on baby monitoring devices for more in depth information.
Concerns of reflux:
Reflux tends to be common in babies who are born prematurely. While there is the likelihood that they will be discharged with medication to help with it, you may still be tempted to elevate their head and chest using a wedge to minimise symptoms.

However, research shows that raising your baby’s head and chest does not reduce reflux or prevent them from choking should they have any spit up or vomit. The reason for this is that babies have a specific reflex which automatically kicks in and causes them to cough or swallow anything that comes up. Therefore their airway is protected should they vomit while lying flat on their back.
What sleep practices in the NICU should not be continued at home?
While in the NICU, you may see your baby being placed in various positions while they sleep as well as being cocooned by rolled up blankets and towels. This is to help mimic the womb-like environment as well as to try and maintain the flexed position which is how they would be in your womb if they were not yet born. This might lead you to think that it is beneficial for your prem or low birth weight baby and safe to do once you are home. However, in the NICU, your baby is under constant supervision from nursing staff as well as various monitors and intervention can happen quickly should it be needed.
Although allowing your baby to sleep on their tummy as they did in the NICU can assist with digestion and breathing, the risks of SIDS and suffocation outweigh any benefit. Therefore, once you are home with your baby, it is vital that the safe sleep principles be practiced.

Importance of Kangaroo care with prems and necessary safety precautions:
Kangaroo care allows for skin-to-skin contact with your prem or low birth weight baby and plays an important part in their healing while in the NICU. Not only does it encourage bonding between you and your baby but the warmth of your skin and the sound of your heart beat promotes weight gain, a more consistent heart rate and breathing and allows them to enter a deeper sleep.
It is encouraged that this skin-to-skin time with your baby continues once you are home as the benefits are still evident. However, there are precautions which should be put in place. The most important point is that you are awake and alert while doing kangaroo care. This ensures that you are able to monitor your baby’s breathing and check they do not slip into any positions which could lead to suffocation. Read more in our “Is it safe for my baby to sleep on my chest” blog for more information.

Although it can be overwhelming, it is important not to lose sight of the fact that your baby would not have been discharged from the NICU if they were not yet ready. Making use of safe sleep practices can reassure you that you are doing your best to keep them safe.
references
https://www.marchofdimes.org/complications/preterm-labor-and-premature-birth-are-you-at-risk.aspx
https://adc.bmj.com/content/99/Suppl_2/A544.2
https://www.marchofdimes.org/complications/low-birthweight.aspx
https://pediatrics.aappublications.org/content/pediatrics/120/6/1390.full.pdf
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2780991/
https://kidshealth.org/en/parents/preemie-home.html
https://www.uptodate.com/contents/image?imageKey=PEDS%2F119362&topicKey=PEDS%2F4992&source=see_link
Our Products
Precious Cargo is a proud stockist of certified Safe Sleep products in South Africa. Feel free to contact us for more information on our products.

